Clear Notes
Structured progress notes for behavioral health teams
Clear Notes transforms documentation into a guided workflow. Clinicians select treatment goals, interventions, and client responses—then generate structured, audit-ready progress notes in seconds.
No new system. No data migration. No external PHI storage.
Structured documentation workflow
Clear Notes guides clinicians through structured clinical inputs that connect treatment goals, interventions, and client responses. These selections generate a clear, structured progress note ready for review.
- • Guided clinical inputs
- • Structured progress note generation
- • Consistent documentation format
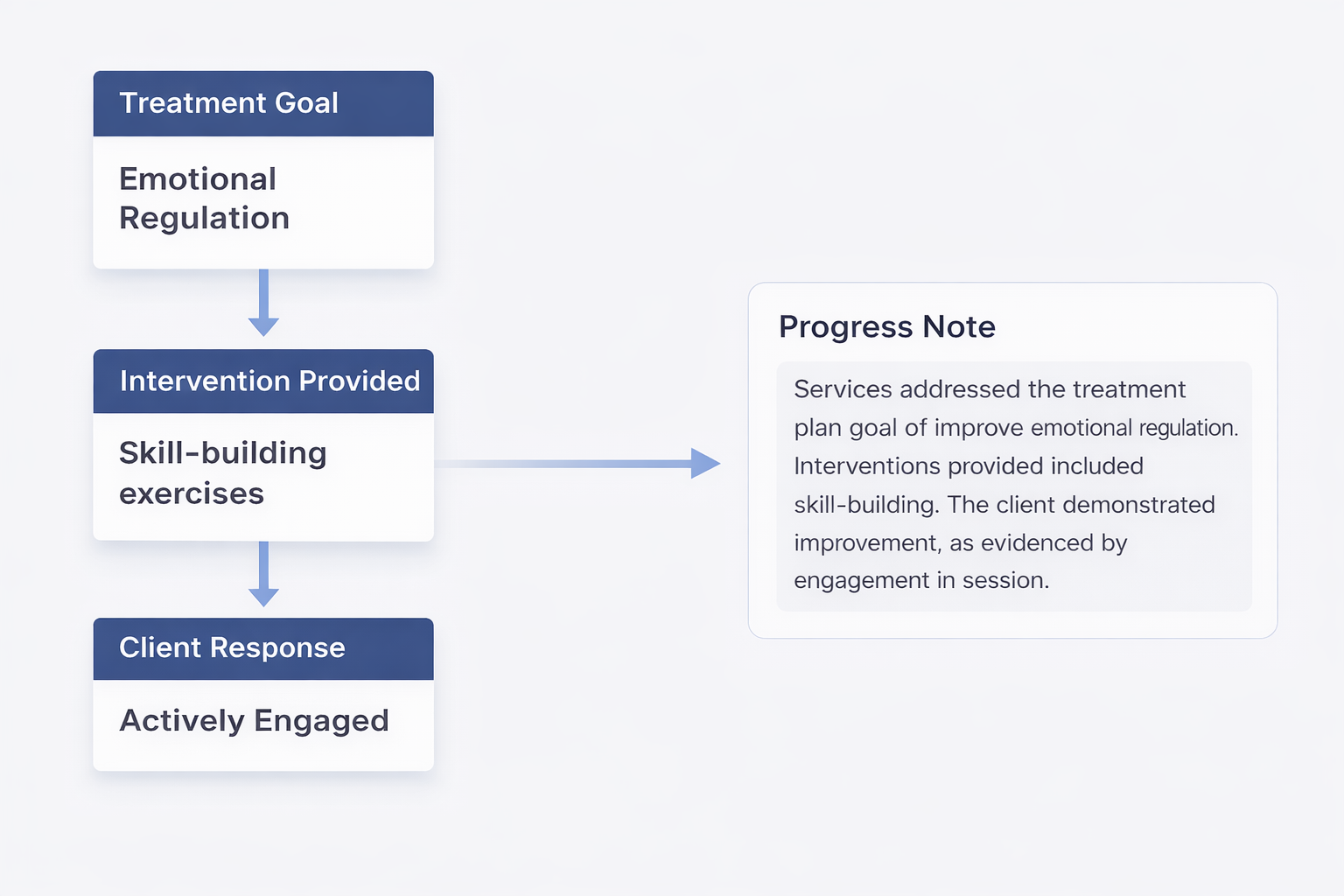
Structured clinical inputs
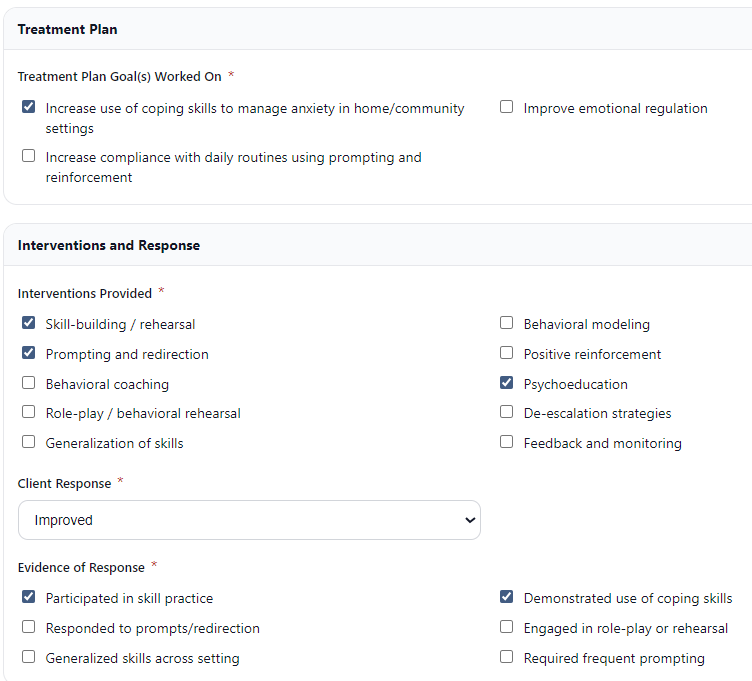
Clinicians complete guided inputs aligned with treatment plans, interventions, and client responses. This structured approach reduces the need for repetitive narrative documentation.
- • Treatment goals selected directly from the plan
- • Intervention and response tracking
- • Evidence of response captured during the session
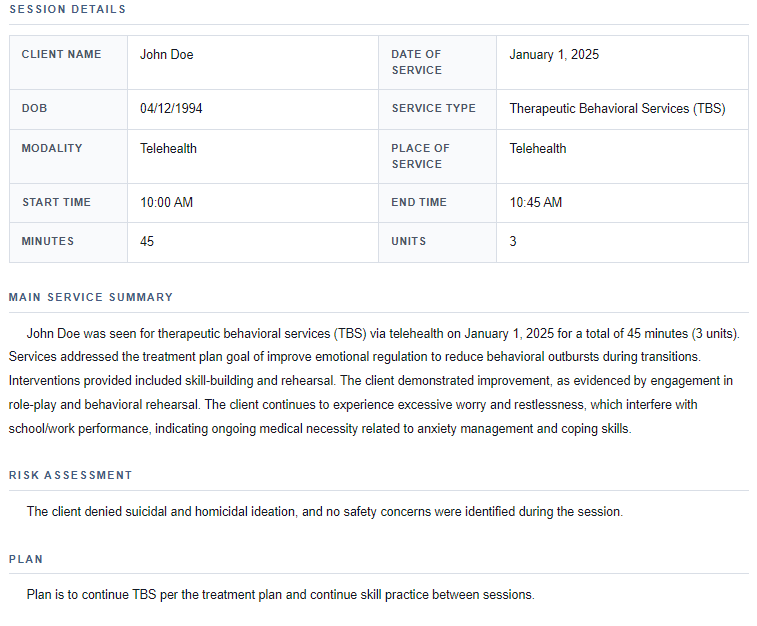
Automatically generated progress notes
Structured responses are transformed into clear progress notes that connect services provided, interventions used, and client progress during the session.
- • Clear clinical documentation
- • Consistent note structure
- • Ready for EHR entry
Simple implementation process
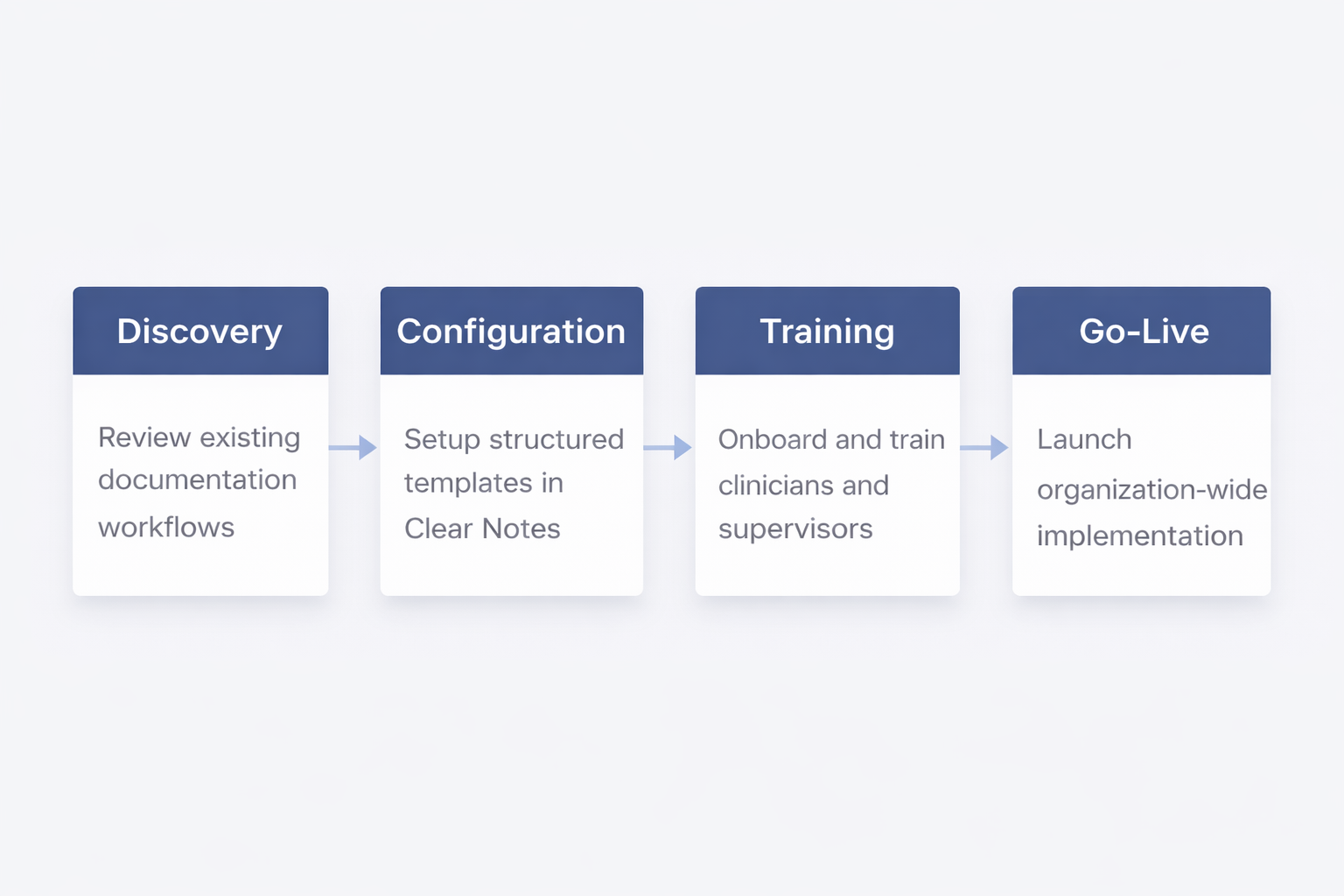
Clear Systems works with organizations to configure Clear Notes to match existing documentation workflows and clinical programs. Implementation focuses on practical setup and clinician adoption.
- • Discovery of existing workflows
- • Structured template configuration
- • Clinician training and onboarding
- • Organization-wide rollout
See the operational impact of Clear Notes
Clear Notes helps behavioral health organizations reduce documentation time, return capacity to clinicians, and improve consistency across progress notes inside SmartCare.
Estimate your impact
- • 5 notes/day
- • 5 min saved/note
- • 48 weeks/year
- • $35/hr cost
Conservative estimate. Actual impact varies.
For a 150-clinician organization:
Annual Savings
$525,000
Hours Returned
15,000
Clinical Capacity Returned
7.2 FTE
(~7 clinicians)
Audit Ready
Structured Notes
More consistent documentation
Watch the workflow in action
See how guided clinical inputs turn into a structured behavioral health progress note. This demo highlights how Clear Notes supports clearer documentation, stronger consistency, and a more efficient workflow.